Background:
Stereotactic radiotherapy (SRT) is a non-invasive treatment modality that is currently evaluated for use in renal cell cancer (RCC). We aimed to evaluate current utilization of SRT for stage I RCC and compare associated overall survival with thermal ablation (TA) and partial nephrectomy (PN).
Methods:
The 2004-2015 United States National Cancer Database was searched for histopathologically approved stage I RCC treated with PN, cryoablation (CRA), radiofrequency- or microwave-ablation (RFA/MWA) or SRT. Patients were propensity score matched to account for potential confounders. Overall survival (OS) was evaluated with Kaplan-Meier plots, log-rank tests and Cox proportional hazards models.
Results:
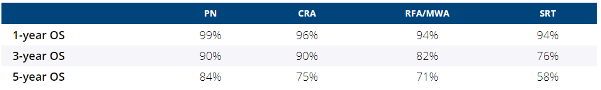
A total of 91,965 patients were included (SRT n = 174; PN n = 82,913; CRA n = 5,446; RFA/MWA n = 3,432).Stage I SRT patients tended to be older females with fewer comorbidities and treated at non-academic centers in New England states. After propensity score matching, a cohort of n = 660 patients was obtained with well-balanced distribution of confounders between the different treatment strategies. In the matched cohort, OS following SRT was inferior to PN and thermal ablation (PN vs. SRT HR = 0.33, 95% CI: 0.22-0.50, p < 0.001; CRA vs. SRT HR = 0.44, 95% CI: 0.30 – 0.66, p < 0.001; RFA/MWA vs. SRT HR = 0.53, 95% CI: 0.36-0.77, p < 0.001). OS following CRA was comparable to PN (HR = 1.35, 95% CI: 0.84-2.18, p = 0.216), while OS following RFA/MWA was inferior to PN (HR = 1.61, 95% CI: 1.01-2.56, p = 0.046). OS rates are summarized in table 1.
Conclusions:
Only a minority of RCC patients receive SRT. In stage I RCC, current renal SRT protocols yield lower overall survival compared to thermal ablation and resection, while CRA and PN show comparable outcomes. Based on the current body of evidence, SRT for RCC should be reserved for clinical trials or exceptional clinical circumstances.